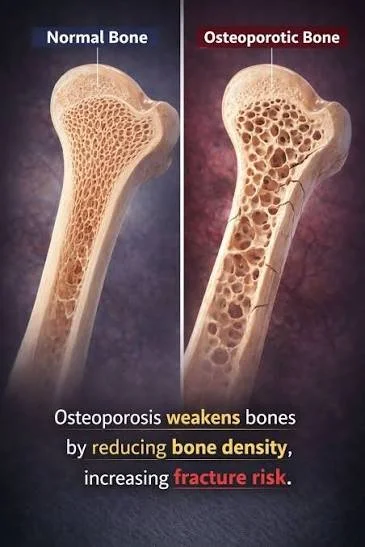
The Hidden Risk of Rapid Weight Loss: What GLP-1 Drugs May Be Doing to Your Bone Density
In the last few years, medications such as Ozempic, Wegovy, and other GLP-1 receptor agonists have dramatically changed the conversation around weight loss. For many people struggling with obesity or metabolic disease, these drugs have offered something that traditional dieting often failed to achieve: significant, sustained reductions in body weight.
The results can be impressive. Individuals frequently report losing 15–20% of their body weight. Blood glucose levels improve, cardiovascular risk markers decline, and the scale moves in a direction that previously seemed unattainable.
Yet beneath these success stories lies a quieter and less discussed question. What happens to the body when weight drops rapidly, particularly when that weight loss occurs without deliberate efforts to preserve muscle and skeletal health?
Weight loss is commonly framed as a universally positive outcome, but human physiology is more complex than the number displayed on a bathroom scale. While reductions in excess body fat can improve metabolic health, the process of losing weight—especially quickly—can also influence muscle mass, nutrient intake, and bone mineral density.
For individuals over forty, and particularly for women approaching or experiencing menopause, this issue deserves careful consideration.
The real conversation is not simply about losing weight. It is about how weight loss occurs and what tissues are lost along the way.
Do GLP-1 Drugs Like Ozempic Reduce Bone Density?
Current research suggests that GLP-1 medications themselves are not directly toxic to bone. However, the rapid weight loss they produce can lead to reductions in bone mineral density if muscle mass, mechanical loading and nutritional intake are not maintained.
Several mechanisms explain this effect. Rapid weight loss reduces the mechanical load placed on the skeleton, particularly in the hips and spine. Bone tissue adapts to loading, and when that load decreases the stimulus for bone maintenance weakens. In addition, weight loss can reduce lean muscle mass and overall nutrient intake, both of which influence bone remodelling.
For this reason, researchers increasingly emphasise that individuals using GLP-1 medications should combine them with resistance training and adequate protein intake to preserve musculoskeletal health.
Why Bone Density Matters More Than Most People Realise
Bone density rarely attracts the attention that body fat percentage or muscle definition receives. It cannot be seen in a mirror, it does not appear on a blood test, and it certainly does not feature in before-and-after transformation photos.
However, bone mineral density is one of the most important predictors of long-term independence and physical resilience.
The skeleton is not an inert structure. It is a living tissue that constantly remodels itself in response to the stresses placed upon it. Cells called osteoblasts build new bone, while osteoclasts break down older tissue. Under normal conditions these processes remain balanced, maintaining strong and structurally sound bones throughout adult life.
When that balance shifts toward bone loss, the skeleton gradually becomes more fragile.
This process often progresses silently over many years. People rarely notice it until a fracture occurs, and by that stage the underlying structural decline may have been developing for decades.
Hip fractures illustrate the seriousness of this issue. Among adults over fifty, hip fractures are one of the leading causes of loss of independence and admission to long-term care facilities. Research consistently shows that up to thirty percent of individuals who suffer a hip fracture die within twelve months of the injury.
These outcomes are not simply the result of broken bones. They reflect the cascade of immobility, loss of function, and medical complications that often follow.
For this reason, bone density is not merely an orthopaedic concern. It is a longevity issue.
The Role of Mechanical Loading in Bone Health
The most powerful stimulus for maintaining bone density is mechanical loading.
Every time we walk, climb stairs, lift an object, or perform a resistance exercise, forces travel through the skeleton. These forces create microscopic stress within bone tissue, which in turn signals the body to strengthen the affected areas.
This principle, known as Wolff’s Law, explains why athletes who regularly train with resistance often develop stronger and denser bones than sedentary individuals.
The opposite is also true. When bones are exposed to less mechanical stress, the body gradually reduces the amount of bone tissue it maintains. The skeleton adapts to the lower demands placed upon it.
Rapid weight loss can therefore alter the mechanical environment of the body in several ways.
First, as body mass decreases, the overall load placed on the skeleton during everyday activities also declines. Carrying less weight means the bones of the hips, spine, and legs experience less stress during walking and movement.
Second, weight loss is frequently accompanied by reductions in lean muscle mass. Muscle contractions generate large forces on bone, and when muscle mass declines, those forces diminish as well.
Together, these factors can reduce the stimulus required to maintain bone density.
Rapid Weight Loss and Bone Mineral Density
A growing body of research has shown that significant weight loss can be associated with reductions in bone mineral density.
This has been observed in several contexts, including:
prolonged calorie restriction
bariatric surgery
aggressive dieting
and rapid pharmacological weight loss
While the exact magnitude of bone loss varies between individuals, several mechanisms appear to contribute.
One factor is the reduction in mechanical loading discussed earlier. Another involves changes in hormonal signalling and metabolic pathways that influence bone remodelling. In addition, weight loss often alters nutrient intake patterns, which may affect the availability of calcium, vitamin D, and protein required for bone maintenance.
The concern is not that weight loss itself is inherently harmful. For individuals carrying significant excess body fat, reducing weight can substantially improve metabolic health and reduce the risk of cardiovascular disease and type 2 diabetes.
The issue arises when weight loss occurs without strategies in place to protect muscle and bone.
Appetite Suppression and Nutritional Intake
GLP-1 medications work primarily by reducing appetite and slowing gastric emptying. As a result, many individuals naturally eat less food without consciously restricting calories.
This appetite suppression is central to their effectiveness. However, it can also lead to unintended reductions in key nutrients.
When food intake drops significantly, several nutritional factors become relevant.
Protein intake is often lower than optimal, particularly for individuals who are not deliberately prioritising high-protein foods. Adequate protein is essential for preserving lean muscle mass during periods of weight loss, and muscle mass plays a direct role in maintaining skeletal strength.
Calcium and vitamin D intake may also decline when individuals eat less dairy, fewer fortified foods, or generally smaller meals. Both nutrients are critical for maintaining bone mineralisation.
Magnesium and other micronutrients involved in bone metabolism may similarly be reduced.
In many cases, individuals celebrating rapid weight loss are unaware that the underlying structural tissues of the body—muscle and bone—may be changing as well.
Why Women Over 40 Face a Higher Risk
The interaction between weight loss and bone health becomes particularly important for women in midlife.
Oestrogen plays a central role in maintaining bone density by regulating the balance between bone formation and bone resorption. As women approach menopause, oestrogen levels begin to decline, accelerating the natural process of bone loss.
During the years surrounding menopause, bone mineral density can decline more rapidly than at any other stage of adulthood.
When rapid weight loss is layered on top of this physiological transition, the combined effects may increase the rate at which bone density changes occur.
Lower mechanical loading, reduced nutrient intake, and hormonal shifts may all converge.
For this reason, women over forty who pursue aggressive weight loss strategies—whether through dieting or medication—should pay particular attention to maintaining skeletal health.
The Metric Most People Are Not Tracking
Modern fitness culture tends to emphasise easily measurable outcomes.
People track their calories, their body weight, their body fat percentage, and often their daily step counts. Progress photos and transformation images dominate social media feeds.
Yet one of the most important health markers remains largely invisible in these conversations.
Bone mineral density.
Unlike body weight, bone density cannot be assessed using a scale or simple biometric device. It requires specialised imaging.
The most commonly used method is a DEXA scan, which provides a precise measurement of bone mineral density in key areas such as the spine and hips. The scan is quick, non-invasive, and widely considered the gold standard for assessing skeletal health.
For individuals experiencing substantial weight loss—particularly those over forty—a baseline DEXA scan can provide valuable insight into their bone health and help monitor changes over time.
Despite this, many individuals pursuing rapid weight loss never evaluate this aspect of their physiology.
Weight Loss Versus Functional Longevity
The goal of health and fitness is often framed narrowly in terms of body weight.
However, long-term health is not defined solely by how light someone becomes.
A lighter body that lacks strength, muscle mass, and bone density may be more vulnerable to injury, falls, and fractures as the decades progress.
By contrast, individuals who maintain strong muscles and dense bones are more likely to remain physically capable and independent well into older age.
The real objective should therefore extend beyond weight loss alone.
It should focus on functional longevity—the ability to move confidently, remain active, and maintain independence throughout the later decades of life.
From this perspective, the quality of the tissues preserved during weight loss becomes just as important as the number of kilograms lost.
Strategies to Protect Bone Health During Weight Loss
Weight loss and skeletal health do not need to be in conflict. With appropriate strategies, individuals can reduce body fat while preserving muscle and bone.
Three approaches are particularly important.
Resistance Training
Strength training is one of the most effective tools for protecting both muscle mass and bone density during weight loss.
Exercises that apply meaningful mechanical load to the skeleton—such as squats, deadlifts, step-ups, and loaded carries—stimulate bone remodelling and encourage the body to maintain structural strength.
Resistance training also preserves lean muscle mass, which helps sustain metabolic rate and functional strength.
Adequate Protein Intake
Ensuring sufficient protein intake is essential when losing weight.
Protein provides the amino acids required to maintain muscle tissue, and muscle contractions generate the forces that stimulate bone adaptation.
For many adults, particularly those over forty, protein intakes of approximately 1.2–1.6 grams per kilogram of body weight per day are often recommended when aiming to preserve lean mass during weight loss.
Monitoring Bone Density
Finally, monitoring skeletal health can provide valuable insight into how the body is adapting to weight loss.
A baseline DEXA scan, followed by periodic reassessment when appropriate, allows individuals and clinicians to detect meaningful changes in bone mineral density and adjust training or nutrition strategies accordingly.
The Bigger Picture
GLP-1 medications have opened an important new chapter in the treatment of obesity and metabolic disease. For many individuals, they represent a powerful tool that can help reduce health risks associated with excess body fat.
However, weight loss should never be viewed in isolation.
The human body is composed of multiple interconnected systems, and changes in one area often influence others. Rapid weight loss may alter not only body fat levels but also muscle mass, nutrient intake, and skeletal health.
The scale may drop quickly, but the real question is what remains underneath.
The ultimate goal is not simply to weigh less.
It is to build and maintain a body that remains strong, resilient, and capable for decades to come.
A body that carries you confidently through your sixties, seventies, and beyond.
Because true success in health and fitness is not measured solely by the number on the scale.
It is measured by how well your body continues to function throughout your life
At Poseidon Performance in Dartmouth, our approach focuses on building strength, preserving muscle and maintaining bone health for the long term.
If you are losing weight, whether through lifestyle changes or medication, structured strength training can play a critical role in protecting your body as the weight comes off.